Introducing Lyme and Eating Disorders
There are quite a few reviews in the medical literature documenting the neuropsychiatric conditions associated with Lyme disease, and most of them include the general category of “eating disorders.” But when I searched the medical database for case histories, I could find only one, published in 1992.
Andrew Pachner and colleagues described a twelve-year-old boy who initially presented with right knee swelling, and tested positive for Lyme disease. (1) He was treated with doxycycline for thirty days and his knee was better. However, two months later he became depressed and restricted his food intake, compulsively exercised, and lost 31 pounds.
He still tested positive for Lyme disease and was treated with intravenous penicillin for two weeks, and soon thereafter he was no longer depressed, he ate normally, and gained weight.
Anorexia Nervosa Case Study
This month I reported on a second case of anorexia nervosa in association with Lyme disease. (2) It is important to distinguish between simple anorexia, or loss of appetite, which is common with many medical conditions and infections, and anorexia nervosa, which is a disorder characterized by the obsessive need to lose weight by refusing to eat.
My patient, Diane, was raised in upstate New York, which is highly endemic for Lyme disease. In fact, she had multiple tick bites as a youngster but no known illness. However, she did have some issues that stood out: at two years old she began screaming and pulling her hair out—a condition termed trichotillomania. This gradually morphed into generalized anxiety and irritability.
When she was 14 years old, Diane had another tick attachment that was not treated, and she developed fatigue, frequent sore throats, impaired cognition, and worsening depression, anxiety and irritability.
When she was 15 years old, she began restricting her food intake and purging after meals. This led to an admission to an eating disorder unit, where she was diagnosed with anorexia nervosa. She went in and out of the inpatient facility and an outpatient eating disorder program five times without success. She was also making serious suicide threats.
Her mother is a savvy nurse, and had her tested for Lyme disease—it was positive.
Dr. Daniel Kinderlehrer
Coinfections Play a Key Role
When I first met Diane, she was 16 years old. She was refusing to eat and had a naso-gastric tube in place through which she received all her calories. She stated that she was still overweight and needed to restrict her diet—she was 5’6” and weighed 125 lbs. The interesting thing about her physical exam was the skin on her thighs—reddish striations that look like stretch marks, but not in the normal skin planes. Diane interpreted these as stretch marks that further supported her belief that she was overweight.
In addition to Lyme disease, Diane tested positive for two tick-borne coinfections, Babesia and Mycoplasma. But in addition, she had a fourth tick-borne infection: Bartonella. She tested negative for this microbe, but the testing is notoriously insensitive. However, the red striations on her legs are virtually diagnostic for that microbe. Check out Figures 1, 2 & 3 for pictures of Bartonella striae.
In a study posted in December, 2020, Ed Breitshwerdt and colleagues described 29 patients with mental health issues who tested positive for Bartonella, 24 of whom developed skin rashes at the same time they developed neuropsychiatric symptoms—most of those skin changes look the same as the ones on Diane. (3) The Bartonella striae are caused by new blood vessel formation in layers of the dermis, and biopsies of the striae have demonstrated Bartonella bacteria. (4)
We treated Diane with three months of intravenous antibiotics and a total of one year of oral antibiotics. Her eating disorder has stayed in remission for three years.
Eating Disorders Are Becoming More Common
Traditionally, the etiology of anorexia nervosa is considered to be a combination of genetic and environmental factors, such as dysfunctional home circumstances, a history of emotional trauma and modern Western culture’s emphasis on thinness.
However, there are several reports in the medical literature that describe the role of infections in the etiology of eating disorders. (5-10) There is also a higher risk of eating disorders in children and adolescents with autoimmune disease. (11)
When you connect infection with autoimmunity, one of the outcomes is autoimmune encephalitis—i.e., Pediatric Acute-onset Neuropsychiatric Syndrome (PANS), which will be the subject of the next blog.
Anorexia nervosa is increasingly common and it is serious—it has the highest mortality of any “psychiatric” disorder. Wouldn’t it be great if we could test all the folks who are diagnosed with anorexia nervosa for infections?
Bartonella Gives Warning Signs
Figure 1
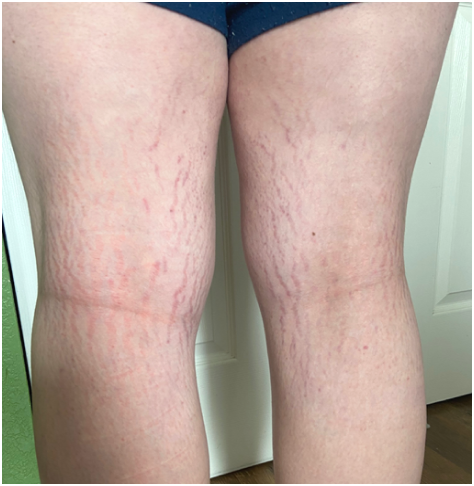
Figure 2
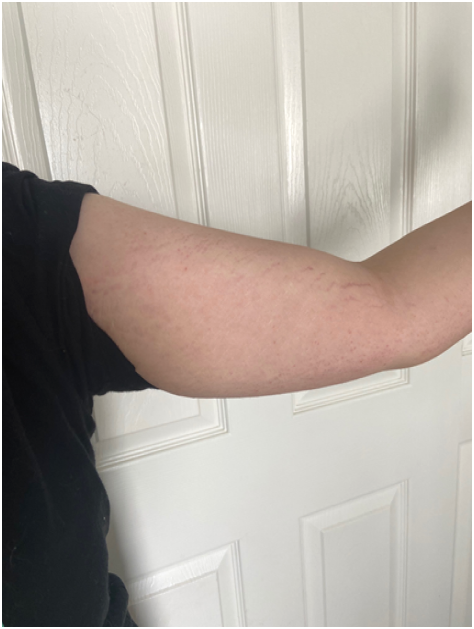
Figure 3
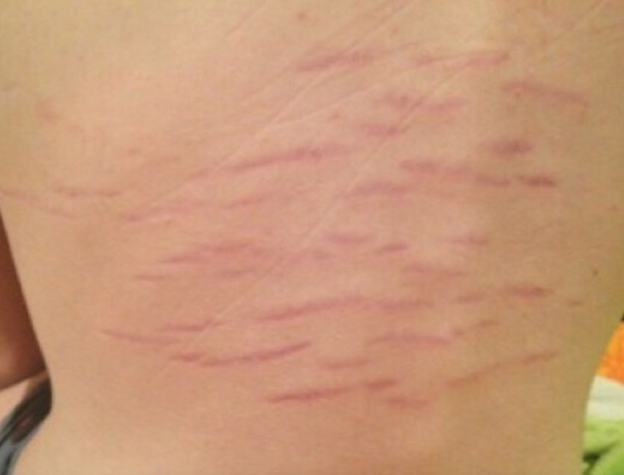
About the Author
Daniel Kinderlehrer, MD, is a nationally recognized physician with expertise in the fields of nutrition, allergy, environmental medicine, Lyme disease, and the healing of mind-body-spirit as a unified whole. He recently released a new book Recovery from Lyme Disease, The Integrative Medicine Guide to Diagnosing and Treating Tick-Borne Illness. The book discusses his integrative approach and offers the most up-to-date and comprehensive plan available for treating and beating this disease
Sources
- Pachner AR, Duray P, Steere AC. Central Nervous System Manifestations of Lyme Disease. Arch Neurol. 1989;46(7):790-795.
- Kinderlehrer, D.A. Anorexia Nervosa Caused by Polymicrobial Tick- Borne Infections: A Case Study. Int Med Case Rep J. 2021;14:279-287.
- Breitschwerdt EB, Bradley JM, Maggi RG, Lashnits E, Reicherter P. Bartonella Associated Cutaneous Lesions (BACL) in People with Neuropsychiatric Symptoms. Pathogens. 2020;9:1023.
- Maluki A, Breitschwerdt E, Bemis L, et al. Imaging analysis of Bartonella species in the skin using single‐photon and multi‐photon (second harmonic generation) laser scanning microscopy. Clin Case Rep. 2020;8(8):1654-1570.
- Brown RF, Bartrop R, Beumont P, Birmingham CL. Bacterial infections in anorexia nervosa: delayed recognition increases complications. Int J Eat Disord. 2005;37(3):261-265.
- Favaro A, Tenconi E, Ceschin L, Zanetti T, Bosello R, Santonastaso P. In utero exposure to virus infections and the risk of developing anorexia nervosa. Psychol Med. 2011;41(10):2193-9.
- Raevuori A, Lukkariniemi L, Suokas JT, Gissler M, Suvisaari JM, Haukka J. Increased use of antimicrobial medication in bulimia nervosa and binge-eating disorder prior to the eating disorder treatment. Int J Eat Disord. 2016;49(6):542-52.
- Park RJ, Lawrie SM, Freeman CP. Post-viral onset of anorexia nervosa. Br J Psychiatry. 1995;166(3):386-9.
- Simon MW. Anorexia and failure to grow associated with Epstein-Barr virus infection. J Ky Med Assoc. 1998;96(1):13-15.
- Breithaupt L, Köhler-Forsberg O, Larsen JT, et al. Association of Exposure to Infections in Childhood with Risk of Eating Disorders in Adolescent Girls. JAMA Psychiatry. 2019;76(8):800–809.
- Zerwas S, Larsen JT, Petersen L, et al. Eating Disorders, Autoimmune, and Autoinflammatory Disease. Pediatrics. 2017;140(6):e20162089.






