Assistance
Other Tick-Borne Diseases
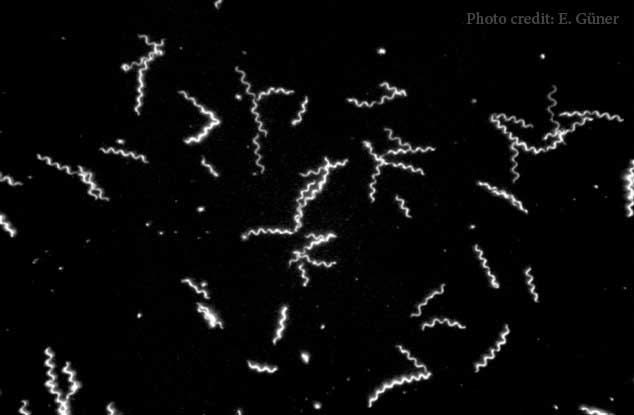

Borrelia Miyamotoi
Borrelia miyamotoi is a spiral-shaped bacteria and a close relative to the bacteria that causes tick-borne relapsing fever (TBRF) in the United States. It’s also a distant relative to Borrelia burgdorferi, the bacteria responsible for Lyme disease. Researchers first discovered B. miyamotoi in Japan in 1995, but it wasn’t found in the United States until 2013. Many of its symptoms overlap with Lyme, but a key differentiator is that it’s rarely associated with a rash. Ticks may pass B. miyamotoi to their offspring, so the infection can be found in tick larva, the early stage of a tick’s life cycle after it hatches from an egg.
Main symptoms: fever, fatigue, headache, chills, muscle aches, joint pain
Types of ticks: blacklegged deer tick, Western blacklegged tick
Borrelia Mayonii
Borrelia mayonii, a species of Borrelia discovered by scientists at the Mayo Clinic in 2013, is the second species in the United States known to cause Lyme disease. It’s most commonly found in the upper Midwestern states, including Minnesota and Wisconsin. While there are many similarities between B. mayonii and B. burgdorferi, a few differences have emerged. For example, B. mayonii may be associated with nausea and vomiting. The rashes can also be larger and cover a wider area, and concentrations of the bacteria in the blood may remain higher.
Main symptoms: fever, fatigue, headache, muscle aches, joint pain, arthritis as the illness progresses, gastrointestinal involvement, widespread rashes
Types of ticks: blacklegged deer tick
Colorado Tick Fever
Considered rare, Colorado tick fever (CTF) is a viral infection transmitted to humans from the bite of a wood tick. Several hundred cases of the disease are reported annually throughout the United States and Canada, but actual cases may be misdiagnosed or undiagnosed, according to the National Organization of Rare Diseases (NORD). Some people will experience a “biphasic” fever, where it lasts for several days, abates for several days, and returns a second time for a shorter duration.
Main symptoms: sudden onset, fever, fatigue, headache, chills, muscle aches, joint pain, sore throat, nausea and vomiting, reduced appetite, reddish rash, enlarged spleen
Types of ticks: wood tick
Powassan Virus
Powassan virus has been found in ticks primarily in the upper Midwest and Northeastern states. Research has shown that the virus can be transmitted in as little as 15 minutes. Many people who are infected with the virus don’t show symptoms, as reported by the CDC. In instances where people develop symptoms, Powassan can become life-threatening, resulting in central nervous system involvement and encephalitis. Fatalities happen in 1 out of 10 people infected. Of those who survive, about half will be affected by long-term symptoms.
Main symptoms: fever, weakness, headache, vomiting, encephalitis, cognitive impairment, loss of coordination, seizures, speech difficulties
Types of ticks: blacklegged deer tick, groundhog tick, squirrel tick
Q Fever
Q fever is caused by the bacteria Coxiella burnetii. The primary ways people become infected with the microbe are by inhaling or ingesting contaminated dust or other particles from the waste of infected animals. The bacteria is most commonly found in cattle, sheep, and goats, but researchers have also detected C. burnetii in ticks, allowing for another mode of transmission to humans. C. burnetii poses a threat as a bioterrorism agent, according to the CDC. The bacteria is highly infectious, and it’s immune to heat, drying, and several standard disinfectants. The symptoms of Q fever can range from mild to severe. A small percentage of people who contract the virus develop chronic Q fever months or years after the initial infection. Chronic Q fever can affect one or more of the heart valves (endocarditis) or cause pneumonia, encephalitis, and more.
Main symptoms: fever, fatigue, headache, chills, sweats, muscle aches, digestive changes (nausea, vomiting, diarrhea, or abdominal pain), loss of weight, chest pain, cough (non-productive)
Types of ticks: Lone Star tick, Rocky Mountain wood tick
Relapsing Fever
Several species of Borrelia are responsible for transmitting relapsing fever, a disease with recurring fevers and other symptoms. There are two main forms of the infection: one that comes from ticks, known as tick-borne relapsing fever (TBRF), and another that comes from body lice, known as louse-borne relapsing fever (LBRF). Borrelia species Borrelia duttoni, Borrelia hermsii, and Borrelia parkerii are associated with TBRF, and Borrelia recurrentis is associated with LBRF.
The CDC reports TBRF is most likely to occur in 14 states, including Arizona, California, Colorado, Idaho, Kansas, Montana, Nevada, New Mexico, Oklahoma, Oregon, Texas, Utah, Washington, and Wyoming. LBRF is predominantly found in developing countries, with famine, war, and poverty being significant contributing factors.
Main symptoms: a week-long cycle of high fever, elevated heart rate, and increased breathing rate, followed by significantly lower body temperature and bouts of sweating. Other symptoms include muscle aches, joint pain, and headaches. Without antibiotic treatment, the cycle may continue several times.
Types of ticks: Soft-bodied ticks from the genus Ornithodoros
Southern Tick-Associated Rash Illness
The Lone Star tick can transmit an infection similar to Lyme disease called Southern tick-associated rash illness (STARI). Patients who contract STARI tend to develop a circular bull’s-eye rash around the tick bite approximately 7 days after the infection. While STARI resembles Lyme, laboratory tests don’t help diagnose it because the exact infectious agent responsible for the illness is unknown. However, the bacteria Borrelia lonestari is believed to be one possibility. A STARI diagnosis is based on the clinical presentation, appearance of a rash, geographic location, and proximity to ticks.
Main symptoms: expanding bull’s-eye rash around the site of a tick bite, fever, fatigue, headache, muscle aches
Types of ticks: Lone Star tick
Tick-Borne Encephalitis
Tick-borne encephalitis (TBE) is caused by the tick-borne encephalitis virus (TBEV), an infectious disease affecting the central nervous system. The virus belongs to the family Flaviviridae. It’s transmitted to humans by the castor bean tick (Ixodes ricinus), the main disease-causing tick species found throughout Europe and the species most likely to transmit Lyme disease. Therefore, a person can become infected with Lyme and a coinfection like TBE.
The majority of TBE cases are found in Eastern Europe and Russia, and the illness is similar to the flavivirus in the United States, which is the Powassan virus. Fatalities happen in 1% to 2% of people infected. The infection may result in long-term, permanent nervous system involvement.
Main symptoms: fever, fatigue, headache, muscle aches, nausea, vomiting. After a period of remission, more severe symptoms may develop in some people, including meningitis, encephalitis, and meningoencephalitis (inflammation of the brain and the membrane around it).
Types of ticks: castor bean tick
Tularemia
Tularemia is a serious infection caused by the bacteria Francisella tularensis. The disease is most prevalent in small animals, such as rabbits, hares, squirrels, and muskrats, but it can spread to humans as well. The primary modes of transmission are from deer fly or tick bites, handling infected animals, breathing in contaminated dust or soil, and drinking contaminated food or water. Researchers who work with tularemia in a laboratory are also at risk of contracting the infection.
Approximately 250 cases of tularemia are reported to the CDC each year. However, it’s been found in every state except Hawaii. The highest concentrations of the infection are located in the South Central portion of the United States, the Pacific Northwest, Martha’s Vineyard, and other parts of Massachusetts.
Tularemia infections can range from mild to fatal and occur in several forms, impacting the skin, eyes, lungs, and lymph nodes. A fever is a dominant symptom in all forms of the infection, and it can rise to as high as 104 °F. The primary forms of the disease include:
Ulceroglandular Tularemia
Considered the most common form of tularemia, it occurs after the bite of an infected deer fly or tick or from handling an animal that has been infected with the bacteria. A skin ulcer usually develops at the entry point of the bacteria. In addition to the ulcer, symptoms such as swollen lymph nodes and fatigue may be present.
Main symptoms: a skin ulcer at the site of the infection, swollen lymph nodes, fever, fatigue, headache, chills
Types of ticks: dog tick, wood tick
Glandular Tularemia
The symptoms of the infection are similar to those of ulceroglandular tularemia, but no ulcers are present. Glandular tularemia also comes from the bite of an infected deer fly or tick or from handling an animal that has been infected with the bacteria.
Main symptoms: swollen lymph nodes, fever, fatigue, headache, chills
Types of ticks: dog tick, wood tick
Oculoglandular Tularemia
For this form, the entry point of the bacteria is through the eye. For example, a person who touches their eye after working with an infected animal may contract the infection.
Main symptoms: Pain in the eye, redness, swelling, or discharge of the eye, formation of an ulcer on the eye, light sensitivity
Oropharyngeal Tularemia
The entry point is through the mouth and can be problematic to the mouth, throat, and digestive tract. This form typically results from eating or drinking contaminated food or water.
Main symptoms: sore throat, tonsillitis, ulcers in the mouth, swollen glands in the neck
Pneumonic Tularemia
Entering through the lungs, this form of tularemia is the most severe, according to the CDC. This form can be acquired from breathing in contaminated dust or aerosolized particles. Additionally, if other forms of tularemia aren’t treated, the bacteria may spread to the lungs.
Main symptoms: coughing, chest pain, trouble breathing
Typhoidal Tularemia
Individuals with typhoidal tularemia have a combination of symptoms from other forms, but the infection’s entry point is unknown.
Main symptoms: fever, muscle aches, throat pain, vomiting, enlarged spleen or liver, pneumonia
Tick Paralysis
Tick paralysis isn’t caused by an infectious microbe. It’s caused by a neurotoxin in the saliva of several different species of ticks, and it gets released into the bloodstream during a tick bite. The neurotoxic agent affects the nervous system, causing ascending paralysis. The paralysis begins in the legs and moves up (“ascends”) the body. It may be confused with other neurologic conditions. Cases of tick paralysis are most likely to occur in the Pacific Northwest, the Rocky Mountain region, and the Southeast.
Main symptoms: unsteady gait, weakness in the legs, weakness begins to move up the body. Without prompt removal of the tick, weakness may progress to the trunk and impact the respiratory muscles, becoming life-threatening.
Types of ticks: American dog tick, Rocky Mountain wood tick
Alpha-Gal Meat Allergy
Alpha-gal syndrome is a food allergy to red meat and other mammalian products. The allergy is acquired from the bite of a Lone Star tick. Lone star ticks are found in the Southeast, Eastern, and South Central parts of the country. In recent years, they have also been found in the Northeast.
When a Lone Star tick bites a human, it secretes a sugar molecule known as alpha-gal. For some people, that sugar molecule activates an immune response, and they develop an allergic reaction to a variety of red meat or other food products from mammals, including dairy, pork, venison, lamb, and gelatin. Often, the allergic reaction happens a while after a tick bite and can range from mild to severe anaphylaxis. The symptoms of alpha-gal syndrome may begin 3 to 6 hours after eating a food or substance containing the sugar molecule. Foods such as fish and poultry don’t contain alpha-gal.
Main symptoms: itching, rash, hives, nausea, vomiting, trouble breathing, low blood pressure, feeling faint, abdominal pain
Types of tick: Lone Star tick
Brucellosis
Main symptoms: fever, joint pain and fatigue.
Types of tick: potential capacity of ticks in brucellosis transmission is evidenced by the detection of Brucella in 16 different tick species. The pooled overall prevalence of Brucella in ticks was 33.87% (range: 0.00–87.80%).

